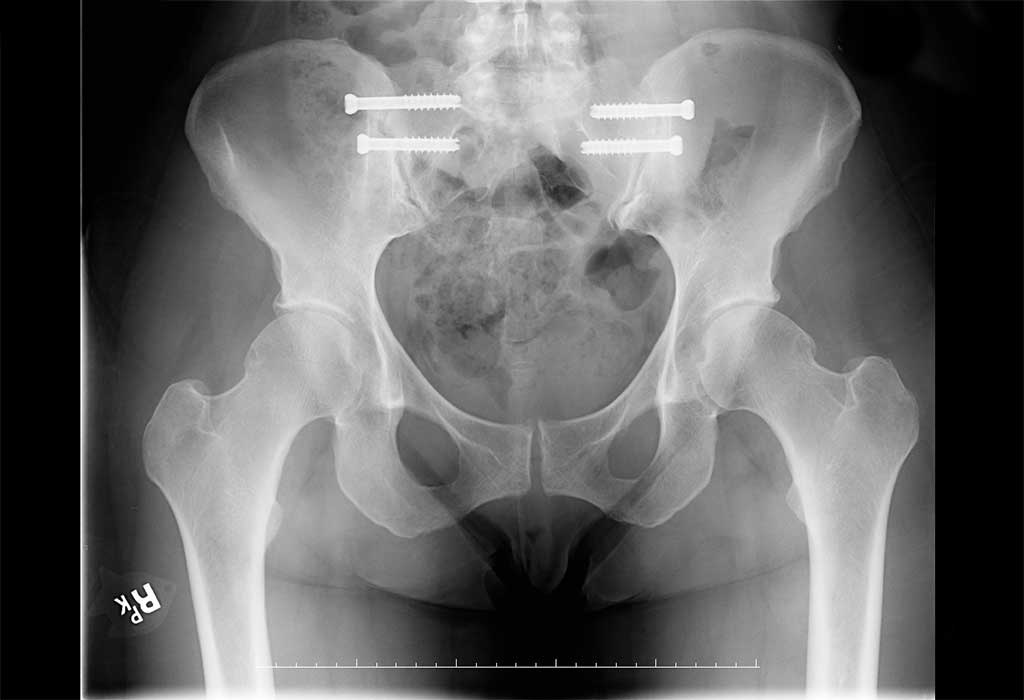
Above featured image displays Bi-Lateral SI Fixation/Pelvic X-Ray at 4 Weeks Post Surgery
The information below offers visitors a quick glance of my personal journey along with the miracles that have brought my life back to wholeness. Through the discovery of practitioners and treatments I have undergone, I finally have relief from the debilitating pain I’ve suffered with for many years. I want to share my story through this website in hopes of helping others who are afflicted as well. This website highlights the following sources of pain:
- Avoid Failed Back Surgery – SI Joint Dysfunction as pain generator – Disorders of Sacrum Diagnosis Code 724.6
- Consider Surgical Procedure Code 27216-50 (bilateral) Defined: Percutaneous skeletal fixation of posterior pelvic bone fracture and/or dislocation, for fracture patterns that disrupt the pelvic ring, unilateral (includes ipsilateral ilium, sacroiliac joint and/or sacrum).
- Stop Chronic SI-Instability with the Percutaneous SI Fixation without fusion Surgery
- Aid in slowing the progression of Lumbar 3-4, 4-5, and L5-S1 Disc Bulges, Fissures, a/o Herniated Discs
- Pirifomis Syndrome – Sciatica Nerve Pain
- Mal-alignment Syndrome – Created by having Chronic SI-Instability
- Neck and Shoulder Myofascial pain to wrist pain
- WWW.FIBULARPAIN.COM Link to full story on the Proximal/Distal Tibiofibular Chronic Instability/Dislocation and the Arthrex Tightrope Dynamic Syndesmosis Stabilization Surgery
- Lateral Knee and ankle pain
- Peripheral Nerve Decompression Neuroplasty for Idiopathic Neuropathy by Surgeon trained at The Dellon Institutes for Peripheral Nerve Surgery
- Commmon (fibular head), Deep (dorsum of foot), and Distal Superficial Peroneal Nerves along with Proximal Tibial Nerve at level of soleus sling
- Fasciotomies – Non-traumatic compartment syndrome
- Subtalar Joint Instability
- My HyProCure Surgery – Extra-Osseous Talo Tarsal Stabilization Minimally Invasive Surgery
- Short Leg Syndrome – Gastroc Equinus and Achilles Tendinitis-Endoscopic Gastroc Recession Surgery
- Impingement Syndrome – Shoulder and ankle
- TMJ – Cranial/Jaw Pain – Adult Orthodontics
- How I’ve Eliminated or Reduced Pain from Head to Toe
The body produces pain for a reason. My integrative medical approach is to share my personal journey so that you may also find the source of your pain, before there is irreversible damage. I have experienced the below associated conditions especially #3,4,5,&6-effects on my discs, muscles, nerves and pubic symphysis.
Common Associated Conditions (quoting with permission from this link):
http://www.sidysfunction.com/common-associated-conditions.php
“Sacroiliac joint dysfunction can occur as an isolated condition, or associated with other spinal disorders.
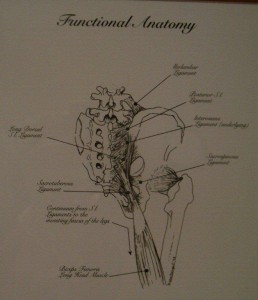
Torsion injuries can cause damage to the disc annulus, facet joints, lamina, pedicle and ligaments, as well as to the sacroiliac joint.
1. FACET JOINT
Torsion or axial rotation causes the facets to flex and laterally bend towards the side of the rotation crushing the facet articular surfaces on the rotation side and distracting the capsule with tearing or avulsion on the side opposite the rotation.
2. NERVE ROOT
The lateral portion of the facet joint is long and slender, making it easily deformed. Torsion causes facet impingement on the torsion side. Distraction on the opposite side can stretch the nerve root. Therefore, neural arch deformation can cause bilateral nerve root entrapment.
3. DISC
Torsion causes annular tears which can weaken the annulus leading to an annular bulge, or herniation, of the nucleolus pulposis.
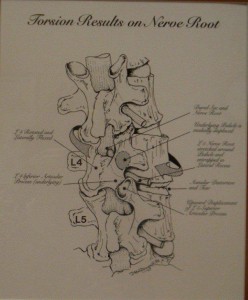
The iliolumbar ligament can become taut due to subluxation of the sacroiliac joint. Its fibers are attached to the transverse process of L4, and chronic tension can lead to bulging of the disc. It is not uncommon to see an L4 annular bulge on the MRI of a patient who has chronic sacroiliac joint instability.
4. EFFECT ON MUSCLE
Janda, an expert on muscle imbalance, has pointed out that postural muscles become facilitated and tighter, and spasic muscles become inhibited and weaker as the result of articular dysfunction. With long-standing dysfunction, anatomic changes in the muscle bundles can take place that are irreversible.
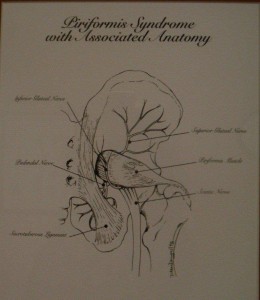
The piriformis is one of the most adversely affected muscle in chronic sacroiliac instability (piriformis syndrome). Pelvic wall muscle spasm, or contracture, may lead to pelvic floor dysfunction. Other muscles affected include the iliopsoas, hamstrings, adductors, gluteus, quadratus lamborum, and the tensor fascia lata.
5. EFFECT ON NERVES
Due to long-standing spasm, or secondary fibrosis, the chronically shortened piriformis can entrap neurovascular structures that accompany it through the greater sciatic foramen (superior and inferior gluteal nerves, the sciatic nerve and the pudendal nerve.)
The lateral femoral cutaneous nerve passes just medial to the anterior superior iliac spine. It can be injured as it passes form the pelvis to the thigh by changes in anatomic positioning associated with sacroiliac joint subluxation (meralgia paresthetica).
6. PUBIC SYMPHYSIS INSTABILITY
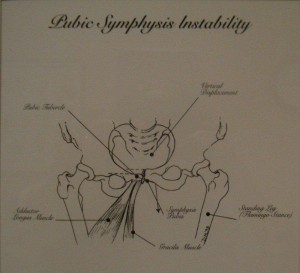
With chronic sacroiliac joint instability the contralateral sacroiliac joint and the pubic symphysis may destabilize.”
Thank you for your visit to SI-Instability.com
If you landed here at SI-Instability.com through your search for relief from your discomfort and affliction and perhaps traditional medical procedures are not relieving your pain, you may wish to click through the various links to find the information you’re seeking. Alternatively, visitors who would like to follow my personal journey from the start may choose to begin here.